Knox Wellness
Center for Integrative Medicine - Knoxville TN
Quick Contact
Social / Phone

Integrative & Functional Medicine
Autoimmune Conditions
Bioidentical Hormones
Diabetes Support
Thyroid Management
Gut Health
Oncology Support
Pediatric Wellness
Autism Support
Lyme Treatment
Mold Treatment
Integrative Oncology and Cancer Support

Comprehensive Therapies
Integrative Oncology Support
Ozone Therapy
Advanced IV Therapy
Advanced Diagnostic Testing
Hormone Pellet Therapy
IV Vitamin Infusions
PRF for Joints
Chelation Therapy
Ketamine Therapy

Cosmetic Medicine
BOTOX®
Collagen PIN
Microneedling
Dermal Fillers
Laser Treatments
Votiva
Collagen Pen
Microblading
Advanced Skin Care Line
Platelet-Rich Fibrin
Here’s How We Do It
Step One:
Schedule an
Essential Wellness
3-appointment
package
Step Two:
During your first
Essential Wellness
appointment, your
provider will help
you select one or
more paths to
wellness that address
your most vital needs
Step Three:
Schedule follow-up
visit to review test
results and discuss
your personalized
treatment plan
Step Four:
Attend follow-up
appointment one
month later to
assess progress and
discuss next steps
Step Five:
Discover the joy
of a happier,
healthier you!
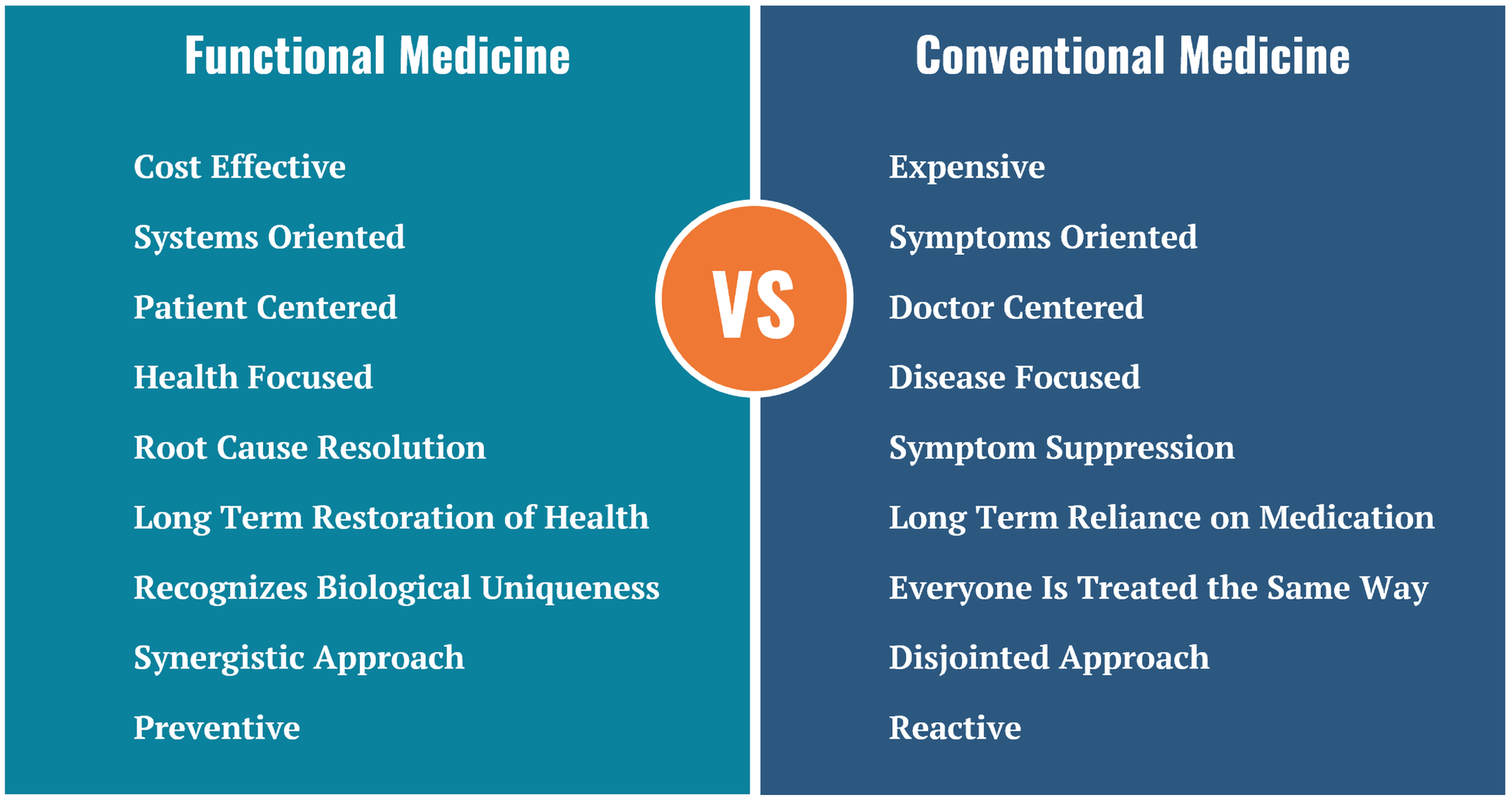

Why Integrative, Naturopathic, Functional Medicine
Why Integrative, Naturopathic,
Functional Medicine
is on the Rise in the U.S.
By Dr. Chris Siano, Medical Director, Knox Wellness Experience
Click here to read
That’s why we’ve dedicated our practice to helping more than 3,000 East Tennesseans get on a path to a healthier life.











